|
Hypercoagulability is a general hematologic concept that merely means an increased risk of thrombosis (i.e., thrombogenic) via enhanced levels of prothrombotic components in the bloodstream. Endothelial wall damage is caused by different factors, which can include direct disruption of the vessel via catheter placement, trauma, or surgery. These three factors are known by the eponym "Virchow's triad." Rudolf Virchow proposed Virchow's triad in 1856, and he described how the presence of these three factors increases thrombosis. Historically, three common factors predispose to thrombosis: 1) damage to the endothelial lining of the vessel wall 2) a hypercoagulable state, and 3) arterial or venous blood stasis. As noted, thrombosis occurs when there is an imbalance in endogenous anticoagulation and hemostasis through a complex pathophysiologic mechanism. The cause of thrombosis is multifactorial. This article will also briefly review the management of venous thrombosis and thromboembolism. This review will focus primarily on the basic pathophysiology of venous and arterial thrombosis, including assessment of provoking risk factors and further workup that may be advisable following the initial presentation. Readers are encouraged to consult additional references for further reading, including regularly-updated subspecialty society guidelines (e.g., American Society of Chest Physicians, American Heart Association, & American Society of Hematology). As such, many of these case- or disease-specific details and management aspects are beyond the scope of this review article. There are also many unique presentations that add complexity to the diagnosis and treatment decisions, such as in acquired antiphospholipid syndrome or with heparin-induced thrombocytopenia & thrombosis (HITT). The state of the science on arterial and venous thrombosis is continually evolving, as is our understanding of provoking risk factors, hypercoagulability testing, and medical management. 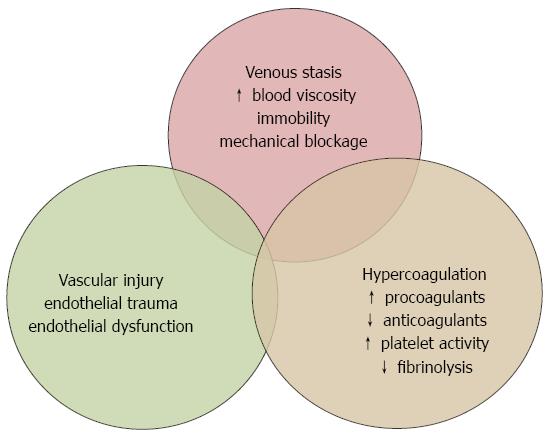
Many patients may require subspecialty evaluation with cardiologists, pulmonologists, neurologists, and/or hematologists. However, the topic is incredibly broad with many management-specific differences and decisions depending on etiology, risk factors, the location of thrombus (venous or arterial), and selection of anticoagulant or antiplatelet therapy. An understanding of the basic pathophysiology of thrombosis and provoking risk factors can aid clinicians in the diagnosis, workup, and management of this condition. This mortality depends on location and acuity of thrombosis, with myocardial infarction and cerebrovascular accident (CVA) or stroke accounting for the highest proportion of thrombosis-associated death in the United States. Together, acute venous and arterial thrombosis accounts for the most common causes of death in developed countries. It should only be completed in carefully selected patients or with subspecialty hematology evaluation prior. Furthermore, a decision to pursue an exhaustive hypercoagulable workup to further evaluate for inherited or acquired conditions that predispose to thrombosis is controversial. The use and duration of anticoagulation or antiplatelet therapy depend on a careful evaluation of these factors. Many factors can impact management decisions, including whether venous or arterial, acute or chronic, first or subsequent episode, family history, risk factor assessment, and hemodynamic stability. They can arise in any organ system, and their clinical presentation can vary depending on underlying comorbidities and presence (or absence) of provoking factors. 
As such, the diagnosis and management of thrombosis are complex. In certain clinical circumstances, patients can be at increased risk of thrombosis and bleeding simultaneously (e.g., disseminated intravascular coagulopathy-DIC, or in patients with underlying malignancy who develop a coagulopathy). When there is an imbalance with this physiologic process, there can be an increased risk of developing a thrombosis versus a coagulopathy (increased risk of bleeding). The ability of blood to flow freely in vessels relies on complex homeostasis that exists between blood cells (including platelets), plasma proteins, coagulation factors, inflammatory factors and cytokines, and the endothelial lining within the lumen of arteries and veins. Thrombosis is the formation of a blood clot (partial or complete blockage) within blood vessels, whether venous or arterial, limiting the natural flow of blood and resulting in clinical sequela.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
